A wrinkle in the retina is a very common problem among older adults. In order to understand what causes this problem and how it can be cured, it is important to learn about the structure of the eye.
The eye is shaped like a small egg and measures about on inch across. The cornea and lens, which lie in the front part of the eye, focus incoming light to form an image on the retina. The retina lines the back wall of the eye and, like the film in a camera, functions to capture and to transmit images to the brain. The central area of the retina where the light is sharply focused is called the macula. The macula allows 20/20 vision and is responsible for reading and other tasks that require fine discrimination. Between the lens of the eye and the retina is a large round space called the vitreous cavity. This space takes up 80% of the volume of the eye and is filled with a gel called the vitreous humor. This gel is normally transparent and is attached to the inner surface of the retina.
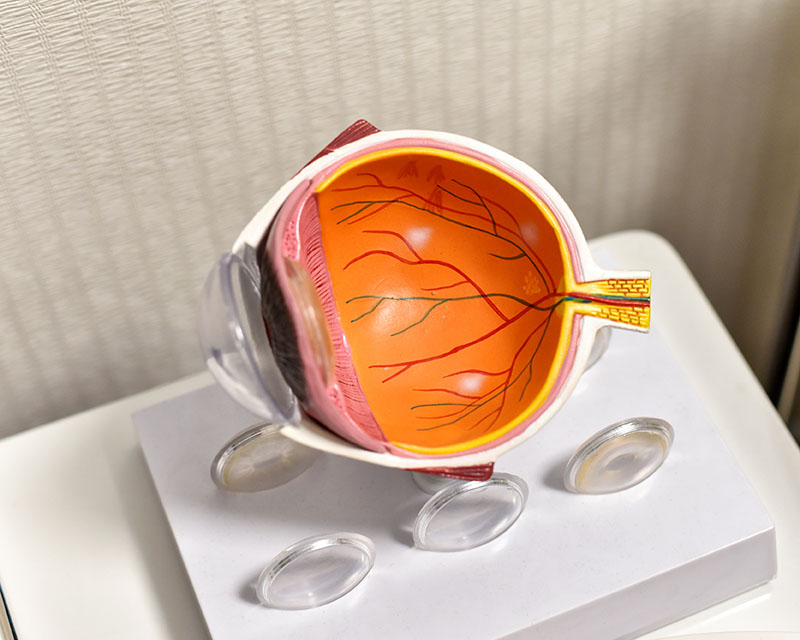
Until a person is about 30 years of age, the vitreous gel has the consistency of raw egg whites. After age 30, the gel undergoes a slow degeneration during which pockets of salt water form inside the gel and it starts to sag. Eventually, so much water forms inside the gel that it cannot support itself anymore and the structure collapses. The collapse of the vitreous gel is called a vitreous detachment. When the vitreous detaches, it can cause, among other things, microscopic damage to the inner surface of the retina, especially in the macula. The retina heals itself by the migration and proliferation of certain cells that normally are found within the retina. In most people, the healing process occurs without any further problems. In some people, the healing process goes “haywire” and results in the formation of scar along the inner surface of the retina.
This scar tissue is called an epiretinal membrane. Once the scar tissue forms, several things can happen. In most people, it grows very slowly and eventually stops. In some patients, the scar tissue continues to grow and begins to pull on the retina. When the scar tissue pulls on the retina, the retina becomes wrinkled. So instead of the retina having a smooth surface like the bottom of a glass bowl, it looks like a rippled potato chip. Epiretinal membranes have several synonyms; cellophane membranes, surface wrinkling retinopathy, macular pucker, or simply, a wrinkle in the retina.

The symptoms that you may experience with a wrinkled retina include blurry vision while reading or driving or distortion of lines that are supposed to be straight. A retina specialist can diagnose a wrinkled retina during a detailed, painless examination of the retina using special lenses and instruments.
In some patients, the doctor will recommend a fluorescein angiogram test to determine whether the scar tissue is distorting the retinal blood vessels so much that fluid leaks from these vessels into the retina. This condition is then called macular edema and poses a more serious threat to vision than if no fluid is present.
What will happen to your vision if you have a wrinkled retina? Fortunately, in most patients, vision is only mildly affected. However, in some patients, the vision can decrease to the level of legal blindness over many months. A wrinkled retina will almost never cause total blindness. Wrinkled retinas can affect both eyes in about 1 out of 10 patients, although one eye is usually worse than the other and both eyes are not usually affected at the same time.

The best way to monitor your vision is to test your eyesight every week with the Amsler Grid that you are given. The treatment that Dr. Kirsch, Dr. Hairston, and/or Dr. Ho recommend for wrinkled retinas is custom designed for your individual situation. If the vision is still good enough for you to read and drive, and the symptoms of distortion are not bothering you very much, conservative observation with very careful regular examinations every 4 to 6 months is usually recommended. The exception to this rule is if there is a significant amount of fluid in the retina found on examination or with the fluorescein dye test. If the symptoms are difficult for you to tolerate or the vision has significantly decreased, then surgery is usually offered as the treatment of choice.
Ophthalmologist smiling after performing surgery. Before discussing surgery, it is important to understand that there are no medications, eye drops, vitamins, or laser treatments that can treat a wrinkled retina. The operation for a wrinkled retina is performed in the regular operation room and can be done under local or general anesthesia. You may go home the same day or stay overnight in the hospital.
The risks of this operation include retinal detachment (occasionally), infection inside the eye (rarely), and bleeding inside the eye (rarely). These complications are treatable most of the time, although as with any surgery inside the eye, loss of eyesight can rarely result. In some patients (about 1%) the scar tissue grows back. If you already have a cataract, surgery will most likely make it worse. The surgery is called a vitrectomy because the vitreous gel inside the eye is removed through 3 small incisions. Each incision is about 1 millimeter in length and is closed with very fine absorbable sutures. The vitreous gel is replaced with salt water (the vitreous is like your appendix; you have it but you are sometimes better off without it). The edge of the scar tissue is then identified and separated from the surface of the retina. Using special microscopic forceps, the scar tissue is peeled from the surface of the retina like you would peel a label from its backing. The surgery for wrinkled retinas is successful in the vast majority of patients, although it can take from 6 to 12 months for the vision to improve. The vision and symptoms in eyes with wrinkled retinas can be improved in 80% to 90% of cases. Working with our specialists, you can decide which course of action is best for your situation to best preserve or restore the precious gift of sight.