
Diabetes mellitus affects approximately 16 million Americans. Diabetes occurs in two main forms: Type I (also called juvenile-onset) in which the pancreas does not produce enough insulin for a person to live; and Type II (also called adult-onset), in which the pancreas continues to produce insulin but the cells in the rest of the body have difficulty using the insulin effectively. Patients with Type I diabetes must always take insulin, while patients with Type II diabetes may be treated with diet alone, pills, and/or insulin.
Although diabetes is a disorder of glucose metabolism, the disease affects many different parts of the body including the eyes. When diabetes affects the eyes, the most serious problems are found in the retina. This complication of diabetes, called diabetic retinopathy, is the leading cause of new blindness in the United States among people aged 25 to 64 years.
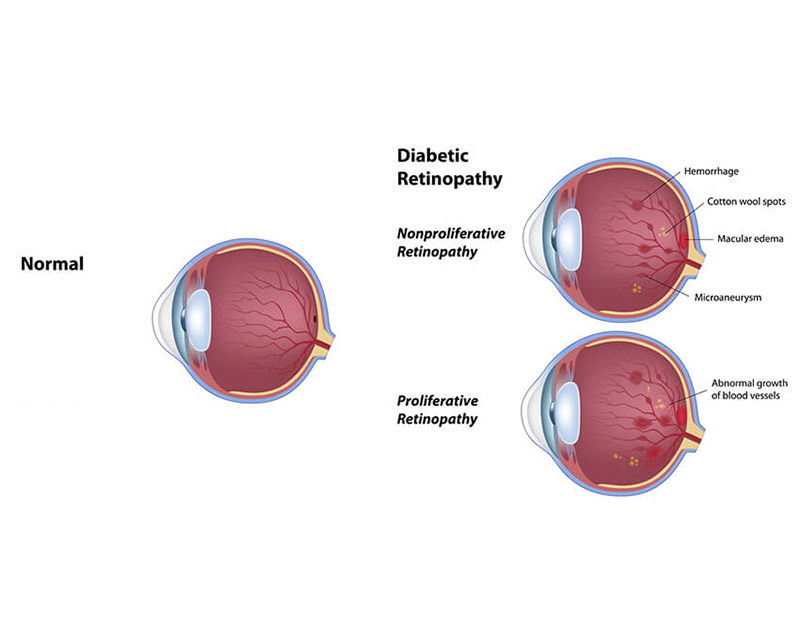
The retina is a transparent layer of tissue that lines the back wall of the eye like a piece of wallpaper on a wall. The retina functions, as does the film in a camera, to take the light coming into the eye and make a “picture” that is sent to the brain. The very center of the retina is called the macula. The macula is the part of the retina that allows the eye to have 20/20 vision. The retina is nourished by many small blood vessels that are damaged after a person has diabetes for several years, especially if the blood glucose is poorly controlled.
In proliferative diabetic retinopathy, the blood vessels supplying the retinal tissue become so damaged they lose the ability to adequately nourish the retina. The eye responds to this situation by increasing the production of vascular endothelial growth factor (VEGF) which starts the process of growing new blood vessels. Unfortunately, these new blood vessels grow or “proliferate” (hence the term proliferative retinopathy) along the surface of the retina and do not actually meet the need for more nourishment of the retina. The abnormal new blood vessels can cause two major problems leading to loss of vision. They are very fragile and can easily break, causing hemorrhage into the large cavity in the back part of the eye. The blood vessels can also eventually form large sheets of scar tissue that can pull on the retina and lead to a retinal detachment. These two problems often have to be corrected by advanced microsurgery performed in the operating room.
The main goal of treating proliferative retinopathy is to prevent the new vessels from causing hemorrhage or a retinal detachment. This greatly reduces the risk of permanent severe vision loss, as well as, the need for major surgery. By carefully examining the retina, your surgeon can detect the new blood vessels growing on the retina before they cause a major problem. If new blood vessels are detected, laser treatment is usually recommended. The laser treatment is different than the laser performed for macular edema. In proliferative retinopathy, up to 2,000 laser spots are placed around the front part of the retina, away from the macula. This procedure is also done in the office and may be divided into two treatment sessions scheduled one week apart. Some mild discomfort may be felt for a few days afterward. The other common side effect is a mild decrease in the “side” or peripheral vision, especially at night. The new blood vessels begin to shrink within a week of the treatment. Additional laser treatment can be performed if the blood vessels don’t regress entirely or if they come back. In most patients, laser treatments cure the problem of proliferative retinopathy permanently.
Recently, there has been a great deal of research regarding the use of medications that inhibit vascular endothelial growth factor (VEGF) to treat both macular edema and proliferative diabetic retinopathy. VEGF is a family of 6 proteins produced all over the body, including in the eye, that are critically important in the development of both normal and abnormal new blood vessels. In diabetic retinopathy, VEGF is produced in abnormally high amounts and leads to the leakiness of the macular blood vessels. This production, in turn, causes macular edema and also causes the formation of the abnormal new blood vessels that arise in proliferative diabetic retinopathy.
All anti-VEGF treatment is administered as an injection into the vitreous cavity, which is a procedure performed in the office. The surface of the eye is numbed with drops and then an anesthetic injection of lidocaine is given under the conjunctiva (the “skin” covering the white part of the eye). The eye is then thoroughly cleaned and sterilized with betadine and antibiotic drops. The anti-VEGF medication is injected through the anesthetized area into the vitreous cavity using a very tiny needle. The procedure itself is painless and straightforward. However, it is considered an invasive procedure because we are entering the eye itself and there is a rare chance of complications, such as cataract, retinal detachment, bleeding or infection. These complications occur less than one in a thousand injections. Occasionally, the volume of medication injected temporarily interrupts the circulation to the eye, and it might be necessary for the surgeon to remove some fluid from the front of the eye to restore the normal circulation. All patients receiving an injection are asked to take antibiotic drops for four days after the injection to lessen the chance of infection. These injections are usually repeated every 4 to 6 weeks as necessary until the problem is resolved.
There are three anti-VEGF medications that may be used to treat diabetic retinopathy: Avastin, Lucentis, and Macugen. None of these medications are approved by the Food and Drug Administration to treat diabetic retinopathy. Lucentis and Macugen are approved for treating wet macular degeneration, while Avastin is used “off-label” for all eye diseases. There has been some encouraging news lately regarding the effectiveness of these medications. In practice, Avastin is normally used because of the issues of cost; it is significantly less expensive. It is also as or more effective than either Macugen or Lucentis.

There are two aspects of the care of diabetics which deserve special recognition. The first is the family doctor, internist, or endocrinologist responsible for managing your diabetes sends you to an ophthalmologist at least once a year for a retinal examination; if your doctor does not suggest this to you, ask him for a referral. Early detection of macular edema or proliferative retinopathy leads to a much better chance of keeping your eyesight.
The second issue revolves around strict control of blood sugar. The results of a study called the Diabetes Control and Complications Trial, for which Dr. Kirsch was a co-investigator, were first published in 1993. This study conclusively demonstrated that Type I diabetics, who very strictly controlled their blood glucose, had a delay in the onset of any form of diabetic retinopathy. Furthermore, if there was already some damage to the retina, the progression of retinopathy was significantly slowed by keeping the blood sugar as close to normal as possible. We now believe all diabetics should monitor their blood sugar frequently, adhere to a strict diet, exercise regularly, and try to tightly control their blood sugar levels.
While diabetes cannot be cured at the present time, it can be controlled. Most of the retinal problems caused by diabetes can be detected in the early stages and successfully treated. Working together with your primary doctor, can help to preserve the precious gift of sight for a lifetime.