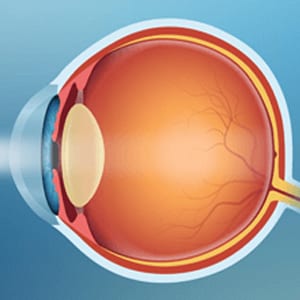
 A cataract is the clouding of the eye’s natural lens, located behind the iris (the colored part of the eye). A healthy lens bends light rays in a way that allows us to form a clear image and focus on objects at various distances. Cataracts compromise this clear vision.
A cataract is the clouding of the eye’s natural lens, located behind the iris (the colored part of the eye). A healthy lens bends light rays in a way that allows us to form a clear image and focus on objects at various distances. Cataracts compromise this clear vision.
At some point in our lives, every person develops cataracts. For some, they begin to form as early as their 40s. Others may not develop cataracts until their 70s or 80s. A lucky handful may never experience the symptoms of cataracts. The progression of cataracts varies as well. You might only develop a cataract in one eye. Typically they form naturally; however, other factors, such as previous eye injury, are often associated with cataract development.
The Eye Institute of West Florida is a world-renowned multi-specialty ophthalmology practice at the forefront of industry advancements related to cataract and refractive techniques and technologies. Cataracts are not created equally, and The Eye Institute knows that in order to provide the best visual outcomes for patients, the approach to diagnosing and treating cataracts cannot be either. They believe that the first step in restoring clear vision is assisting patients in understanding the types, symptoms and treatment of cataracts.
There’s more than one type of cataract?
In short, yes.
Director of Cataract and Refractive Services at The Eye Institute, Robert Weinstock, MD explains that, “There are three primary types of age-related cataracts, and as we age, we may develop one type or a combination of the three.”
The most common type of cataract is a nuclear sclerotic cataract, which forms in the central zone of the lens, called the nucleus, and is associated with aging. “Nuclear” refers to the clouding of the central part of the lens, dulling colors, and “sclerotic” refers to the hardening of the central part of the lens, blurring images. Nuclear sclerotic cataracts typically progress slowly and can take years of gradual development before affecting vision.
Cortical cataracts are another common type of cataract. Unlike nuclear sclerotic cataracts, cortical cataracts develop in the cortex, the outside edge of the lens. Cortical cataracts are characterized by white, wedge-like opacities forming from the outside edge of the lens and working their way to the center, creating what looks like the spokes of a wheel. People with diabetes are at higher risk of developing this type of cataract.
The third primary type of cataract is called a subcapsular cataract and forms at the back of the lens. Subcapsular cataracts often affect reading and create halos and glare around lights. This type of cataract often develops more rapidly and is most common is people with diabetes or those taking high doses of steroid medication.
How do I know if I have a cataract?
Similar to cataracts themselves, symptoms vary from person to person.
“A lot of our patients come in thinking they need an updated glasses prescription or confused why their prescription isn’t providing the visual correction they need. This is one of the first signs of cataract development,” Dr. Weinstock notes. He adds, “The majority of cataracts are not visible to the naked eye, so patients aren’t aware that they have developed.”
When cataracts form, images become increasingly blurred, your eyes may become more sensitive to light, creating glare and halos and often impairing night vision, and color contrasts begin to dull.
Dr. Weinstock explains that, “Cataracts typically form gradually and progression can be quite slow. The best way to manage visual changes is with a yearly eye exam.”
Will I ever see clearly again?
Thanks to technological advancements and updates in cataract and refractive treatment techniques, cataract surgery is the safest surgical procedure available. Not only is the procedure itself quick and painless, but the results often leave patients with better vision than they ever had before.
“Cataract surgery today is night and day compared to what our parents and grandparents underwent,” Dr. Weinstock compares, “Today’s procedure takes about ten minutes per eye and the patient is able to go home almost immediately after and can return to typical daily activities within a day or so. There are options available for the procedure to be completely bladeless, making it safer and more precise, we have lasers to break up the cataract and reshape the cornea if needed as well as different lenses available to suit each patient’s individual needs and visual goals.”
Treatment options can seem overwhelming when you do a quick Google search; however, the physicians and team at The Eye Institute of West Florida’s approach to treating cataracts is to get to know each patient. In an initial consultation, along with finding out a patient’s visual complaints, they ask questions about the patient’s lifestyle, hobbies and visual goals.
“Once I understand what a patient’s typical day includes – reading, using the computer, playing golf – combined with the different tests we perform to check the health of a patient’s eyes, I am able to recommend the best option for them. The treatment plan is a decision we make together. It’s essential that I understand their lifestyle and visual goals because often times a patient comes in having done their research and wanting a specific lens when in reality it won’t yield the results they are looking for,” Dr. Weinstock elaborates.
Cataracts are inevitable, but fortunately, we live in a time when technology and treatment options are so advanced that removing cataracts and improving vision is not only possible but safe and painless as well.

